27900 New Market Rd, Farmington Hills, MI 48334
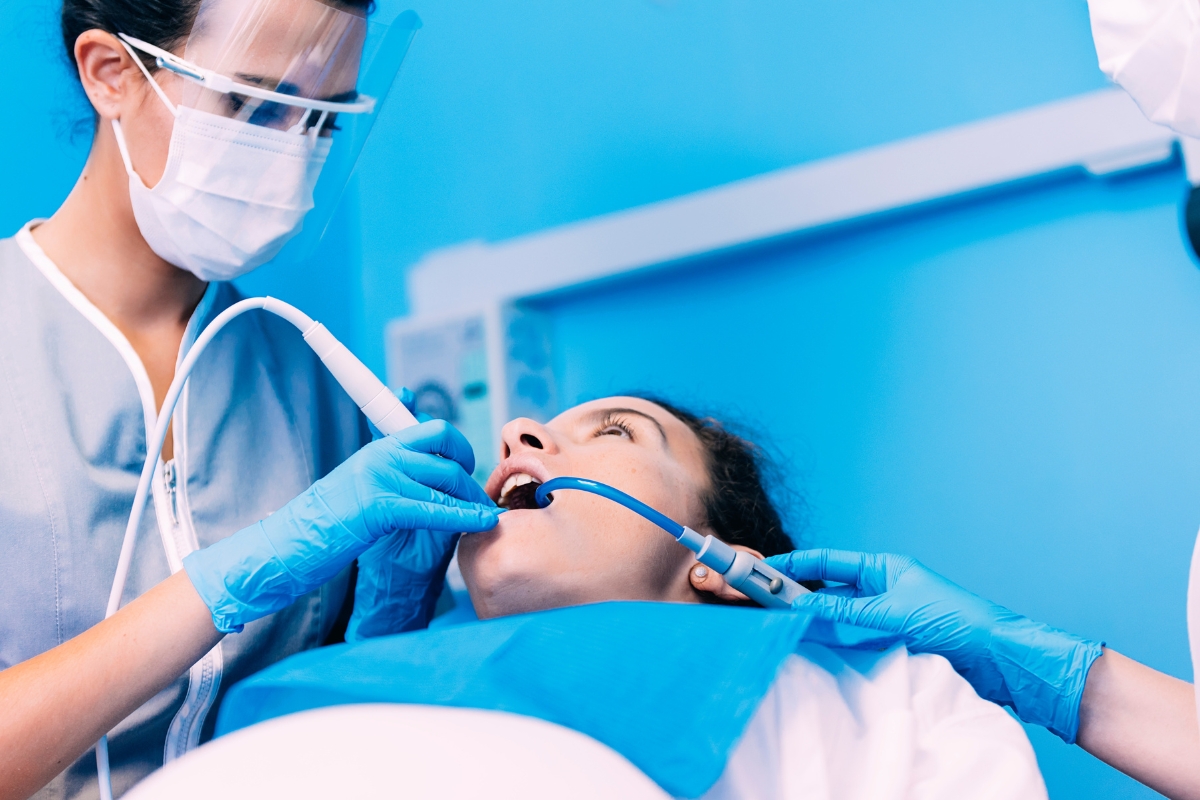
Sedation dentistry has made dental care genuinely accessible for people who previously avoided it — whether because of anxiety, a strong gag reflex, or the need for complex procedures that are more manageable when you’re deeply relaxed. But sedation isn’t simply pressing a button and tuning out. It’s a medical intervention, and like any medical intervention, its safety depends heavily on what your provider knows about you beforehand.
The intake process before sedation isn’t paperwork for its own sake. Every question on that health history form exists because sedating agents interact with the human body in specific ways, and those interactions change depending on your health status, your medications, and your history. Being thorough at this stage isn’t just good practice. It’s what makes the procedure safe.
Why Your Medical History Changes Everything About Sedation
Sedation agents — whether nitrous oxide, oral sedatives, or IV sedation — all affect your central nervous system, cardiovascular function, and respiratory rate to varying degrees. A patient with well-controlled blood pressure responds very differently to the same sedative dose as someone whose hypertension is poorly managed. A patient on certain antidepressants may metabolize sedatives at a different rate than someone not on any medication. These aren’t minor variations — they determine dosage, monitoring intensity, and in some cases, whether a particular sedation method is appropriate at all.
This is why a thorough pre-sedation consultation is standard practice at our office. The sedation dentist in Farmington Hills at our practice reviews your full health picture before recommending any sedation approach because the right option for you depends on factors that go well beyond dental anxiety.
Think of the medical history review less as a formality and more as the foundation of your care plan. What you share and how completely you share it — directly shapes how well your provider can protect you throughout the procedure.
Cardiovascular and Respiratory Conditions
Heart and lung health are among the most critical disclosures before dental sedation. Sedative agents lower blood pressure and slow breathing. For most healthy patients, these effects are mild and carefully monitored. For patients with underlying conditions, those same effects can become clinically significant.
Heart Conditions to Disclose
Tell your dentist about any history of heart disease, arrhythmia, heart failure, previous heart attack, or pacemaker use. Certain sedation agents can affect heart rate and rhythm — your provider needs to know about existing cardiac issues to select the safest approach and have the right monitoring in place. Even if your condition is well-managed with medication, disclosure matters.
Respiratory Conditions
Asthma, COPD, sleep apnea, and other breathing-related conditions all affect how sedation is administered and monitored. Patients with obstructive sleep apnea, in particular, are at increased risk of airway complications during sedation because the same soft tissue dynamics that cause nighttime obstruction become more pronounced under sedatives. This doesn’t mean sedation is off the table — it means your dentist needs to plan for it explicitly.
Your Full Medication List Including Supplements
This is where patients most often leave gaps in their disclosure, usually because they don’t realize a supplement or over-the-counter medication could be relevant. Nearly everything you take has the potential to interact with sedation agents.
Make sure to include:
- Prescription medications — blood pressure drugs, antidepressants, antianxiety medications, anticoagulants, diabetes medications, thyroid medications, and opioids all have known interactions with sedation agents
- Over-the-counter medications — antihistamines, sleep aids, and even some pain relievers can amplify sedative effects
- Herbal supplements — valerian, kava, St. John’s Wort, and ginkgo biloba can each affect how sedatives work or how your blood clots
- Recreational substances — cannabis, whether used medically or recreationally, affects sedation response; alcohol consumption in the days prior also matters
- Vitamins in high doses — vitamin E and fish oil, which can affect bleeding
The safest approach is to bring a written list of everything you take, including doses and how often. Your provider isn’t there to judge your habits — they need complete information to keep you safe.
Allergies and Prior Reactions to Anesthesia or Sedation
Any known allergies should be disclosed to medications, latex, foods, or any other substances. Some sedation agents contain components that trigger reactions in people with certain allergies, and knowing this in advance allows your provider to choose alternatives.
Prior reactions to anesthesia or sedation are equally important. If you’ve ever experienced unusual prolonged grogginess, nausea, vomiting, or any adverse reaction after a medical or dental procedure involving sedation, tell your dentist before your appointment. Some people are slow metabolizers of certain anesthetic agents — something that’s often only discovered after a previous reaction. That history changes how your provider plans your dosage and recovery monitoring.
Additional Medical History That Affects Sedation Safety
Liver and Kidney Function
Both the liver and kidneys play central roles in metabolizing and clearing sedative agents from your body. Impaired liver function — from conditions like hepatitis, cirrhosis, or heavy alcohol use — can cause sedatives to build up to higher concentrations than intended. Kidney disease similarly affects clearance. Patients with these conditions can still receive sedation, but dosing and recovery monitoring require adjustment.
Neurological Conditions
Epilepsy, Parkinson’s disease, multiple sclerosis, and a history of stroke are all worth disclosing. Some anticonvulsant medications interact with sedatives, and certain neurological conditions affect how patients respond to sedative agents during and after the procedure.
Diabetes
Blood sugar management is directly affected by sedation, particularly when fasting is required beforehand. Patients with Type 1 or Type 2 diabetes need specific guidance on how to manage their medications and meals on the day of sedation. This requires advanced coordination, not a conversation at the chair.
Pregnancy or the Possibility of Pregnancy
Elective sedation is generally avoided during pregnancy, particularly in the first trimester. Nitrous oxide in particular has been studied for potential risks during early fetal development. If there’s any possibility you could be pregnant, disclose it before your appointment — your provider will adjust the care plan accordingly.
Complete Disclosure Makes for Safer, Smoother Sedation
The more completely you share your medical history, the more precisely your provider can tailor your sedation plan. There are no wrong answers on a health history form — only incomplete ones that create uncertainty where there shouldn’t be any.
Schedule your sedation consultation today. Come prepared with your medication list, your health history, and your questions, and leave with a care plan designed for you.
People Also Ask
Ideally, your health history should be submitted or reviewed at a pre-sedation consultation at least a few days before the procedure. This gives your provider time to review potential interactions, consult with your physician if needed, and adjust the care plan before your appointment day.
Tell your provider immediately — before sedation begins. Even on the day of your procedure, disclosing a medication you forgot is always the right call. Proceeding without that information is riskier than a brief delay. Your provider will reassess before moving forward.
Body weight and composition do affect sedation dosing and airway management. Higher BMI is associated with increased risk of airway obstruction during sedation. Your provider will assess this as part of your pre-sedation evaluation and may adjust the sedation approach or recommend additional monitoring.
Fasting guidelines vary by sedation type. Oral sedation and IV sedation typically require fasting for a set number of hours beforehand — usually nothing to eat or drink after midnight. Nitrous oxide has less restrictive requirements. Your provider will give you specific instructions based on your procedure.
For patients with complex medical histories — significant cardiac conditions, poorly controlled diabetes, recent hospitalizations, or complex medication regimens — your dental provider may request a medical clearance from your physician before proceeding. This is a precaution, not a barrier, and it protects your safety.
By Village Family Dentistry
Related Articles
New patients and emergency appointments welcome




